Can Australia's Struggling Universal Healthcare Be Saved?

Perched on the jagged edge of the continent, Victoria Bradley jokingly says that her office offers the most stunning backdrop for her medical practice in all of Australia.
Beyond her window, expansive farmlands transition into rugged coastlines, enclosing a tranquil bay marked with stripes of turquoise and teeming with playful dolphins.
Boasting a population of around 3,000 residents, along with several stores, two roundabouts, and a small hospital, Streaky Bay is a picturesque seaside community.
For Dr. Bradley, however, this is far from the case. As the region’s only full-time physician, she dedicated herself to being effectively on-call around the clock for many years.
Managing both the hospital and the general practitioner (GP) clinic made everyday feel like an endless chase. Rounds at the wards preceded, followed, and even interrupted routine appointments. Lunch breaks remained wishful thinking most days, regardless of how well things seemed to be going. In contrast, challenging days could see unexpected emergencies erupting, intensifying her grueling workload further.
Exhausted, she left her position two years ago, causing the last remaining strand supporting the town's healthcare system to break.

Streaky Bay is at the center of a nationwide issue: insufficient governmental support is worsening the scarcity of essential medical personnel such as Dr. Bradley. This situation has led to extended waiting periods for appointments. Furthermore, physicians are starting to establish their own fee structures, causing patient expenses to rise dramatically.
Once highly esteemed, the comprehensive health care system is now collapsing across all fronts, often surviving only through the determination and efforts of physicians and nearby neighborhoods.
Consequently, an increasing number of Australians, irrespective of their place of residence, are postponing or foregoing the medical care they require.
Ahead of the country's election on May 3rd, health has emerged as a crucial concern for Australian voters, with both prominent political parties pledging significant additional funds running into billions of dollars.
However, according to experts, the proposed solutions act merely as temporary Band-Aid measures, whereas what’s truly necessary are extensive alterations to how the system is financed—reforms that have thus far lacked sufficient political motivation.
Australians believe their nation stands at a critical juncture, needing to determine whether universal healthcare is worth preserving.
The fissures within a 'national treasure'
When Renee Elliott relocated to Streaky Bay, health care wasn't something she had on her radar. However, this changed dramatically for the 40-year-old in 2019 when she discovered a cancerous lump in her breast, followed by another one four years thereafter.
Attending a nearby general practitioner was the smallest issue for her. Since the specialized skills and treatments she required were exclusively available in Adelaide, approximately 500 kilometers distant, Ms. Elliott has devoted countless hours and substantial funds toward obtaining critical medical attention. All this occurred as she balanced caring for her three sons and managing her own enterprise.
Although she managed to recover some of the expenses through governmental programs afterward, this only added to the stress during an already traumatic period—taking a toll financially, emotionally, and physically.
Improving yourself...while also managing everything else proved quite challenging.

When Australia's modern health system was born four decades ago – underpinned by a public insurance scheme called Medicare – it was supposed to guarantee affordable and accessible high-quality care to people like Mrs Elliott as "a basic right".
The health financing system in this country is intricate and jointly managed by state and federal authorities. However, the core idea was that Australians could simply show their distinctive bright green Medicare membership card when visiting a physician’s clinic or hospital, after which the costs would be billed to Canberra. These expenses were covered via rebates sourced from tax revenues.
Patients could opt for fully covered care—essentially free of charge—primarily via the growing public health network, or they could choose substantially discounted treatments from the private healthcare sector, which provided additional advantages and options for those seeking such services.
Medicare quickly transformed into a cherished asset for the nation. The intention behind this setup was to merge the finest elements of the UK’s National Health Service with those of the American healthcare system.
Forty years later, many in the industry believe we're heading towards the worst outcomes from both scenarios.
It's undeniable that Australia’s healthcare system remains far superior to many global counterparts, especially concerning emergency services.
However, at the heart of the current crisis and crucial to this election is the issue of general practitioner services, primarily provided through private clinics. Historically, there has been minimal demand for publicly funded options since most General Practitioners have opted to take Medicare reimbursements as complete compensation.
This situation is becoming less common as physicians argue that these reimbursements have not kept pace with the actual expenses associated with providing medical services. Concurrently, staffing deficiencies remain prevalent even with recruitment initiatives targeting foreign professionals, leading to an increased demand that exacerbates price inflation.
Based on governmental statistics, approximately 30% of patients currently have to cover a "gap fee" for an ordinary physician visit – typically amounting to around A$40 (£19.25; $25.55) from their own pockets.
However, experts believe the actual number may be even greater due to frequent visits from elderly individuals and children, many of whom typically receive services through bulk billing. Additionally, an increasing group of people who do not seek medical care because of rising costs are not included in these figures.
Brisbane electrician Callum Bailey falls into this category.
My mother or my partner keeps pestering me constantly... but I tend to endure everything silently because it's quite costly.
The 25-year-old remarks, "Every dollar really matters at this moment. At my age, I should likely be thriving and searching for a home... but even doing something simple like grocery shopping feels overwhelming."
"[I] just can't keep up."
This is a story that James Gillespie continually heard.
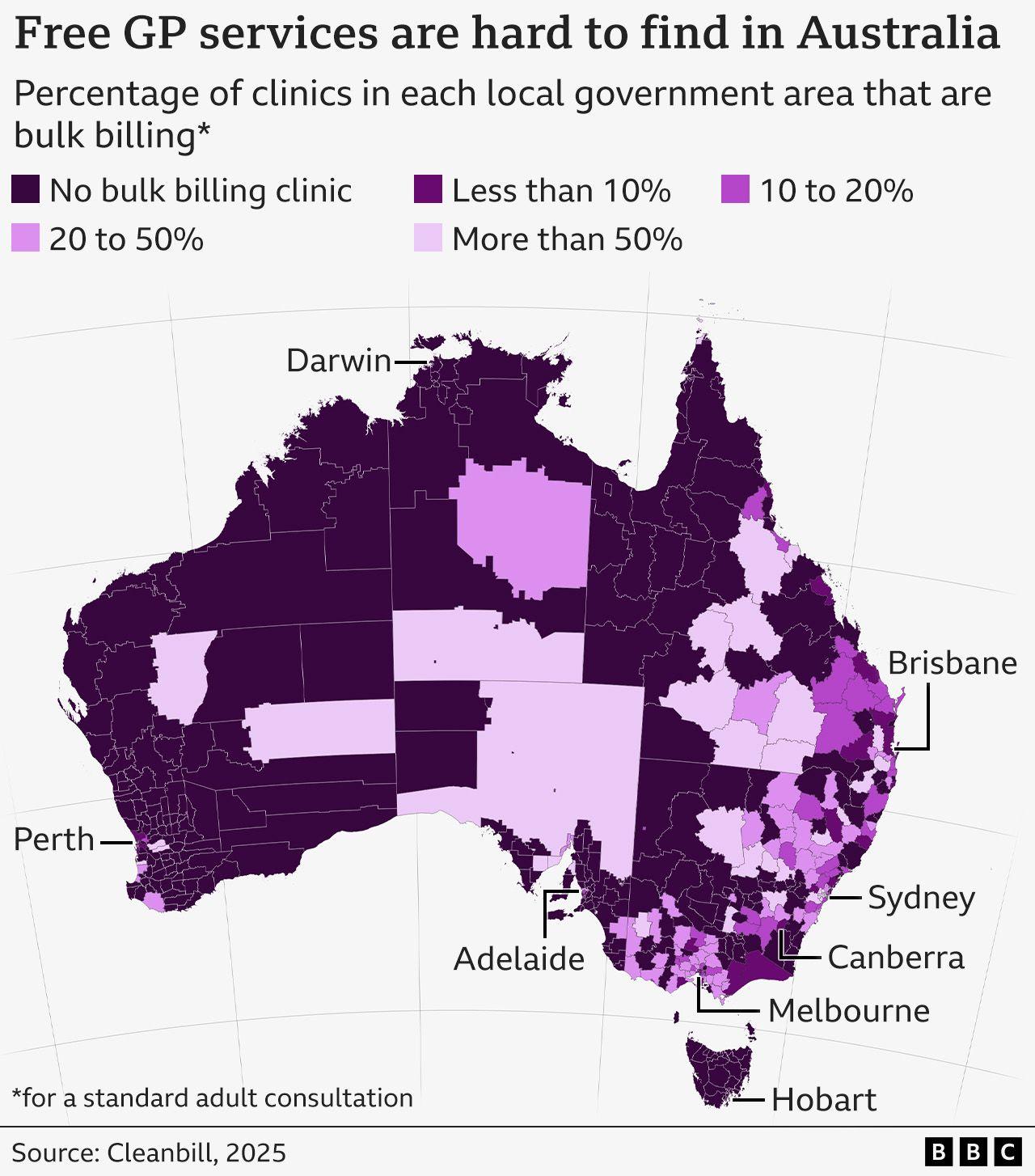
Thus, his venture Cleanbill started pondering this idea: Could an ordinary grown-up in Australia walk into a general practitioner’s office and receive a complimentary basic consultation?
This year, nearly all of the approximately 7,000 GP clinics across the country were contacted—only one-fifth agreed to bulk-bill new adult patients. For instance, not a single clinic could be found in the whole state of Tasmania.
The results resonate with many Australians, he says: "It really brought it home to them that, 'Okay, it's not just us. This is happening nationwide'."
That's merely the start when it comes to primary care.
Public experts are extremely scarce and overburdened – with waiting periods frequently exceeding safe limits – leading most patients to be directed towards highly costly private services. This also applies to numerous non-urgent hospital procedures or dental treatments.
Currently, there are no limits on what private practitioners, dental professionals, or medical facilities may charge. Neither private health insurance nor the limited Medicare rebates consistently provide significant financial assistance.
Priced out of care
They talked to individuals nationwide who claim that the rising expense of healthcare has forced them to depend on charitable organizations for meals, forego dental services for nearly ten years, or deplete their retirement funds to cover medical costs.
Other individuals are resorting to borrowing money from their parents, obtaining payday loans for medications, refinancing their homes, or selling off their belongings.
Kimberley Grima often stays up late at night, mentally sorting out which of her three children – each suffering from chronic illnesses just as she does – can make appointments with their specialists. She rarely gives much thought to her own delayed medical examinations and tests.

"The choices they face aren’t ones anyone would wish upon them," says an Indigenous woman from New South Wales speaking to the publication.
However, when it really comes down to it and you lack the funds... you have no alternative. It's devastating.
A different woman shares that if she could have afforded earlier medical visits, her multiple sclerosis—a progressive nervous system disorder—would have been detected and managed more rapidly.
"I was so disabled by the time I got a diagnosis," she says.
Experts say those who need it the most are often the ones left behind.
"We have much more care in healthier, wealthier parts of Australia than in poorer, sicker parts of Australia," Peter Breadon, from the Grattan Institute think tank says.
This entire situation spawns a self-perpetuating cycle that adds further strain to an overburdened system, deepening inequality and escalating mistrust.
Each and every one of those problems is intensified in the regions.
Streaky Bay has bid farewell to the idea of affordable healthcare for a long time, now struggling merely to maintain access to some form of care.
That's why Dr. Bradley remained for just three months after resigning before "remorse" compelled her to return to practicing medicine.
"There's a connection that goes beyond just being the GP... You are part of the community.
I sensed that I had disappointed them, which is why I couldn't simply move on.


She returned to a much more sustainable three-day workweek at the GP clinic, where Streaky Bay had to compete in a bidding war with other needy areas to attract expensive, fly-in-fly-out doctors to cover the remaining shifts.
This is just another entry on the ledger for a community that has already poured substantial funds from its coffers to support a healthcare system meant to be sustained through state and private investments.
Penny Williams, who assists in managing the community organization owning the GP practice, states, 'Our aim isn’t for a premium service; rather, we desire one that is fair and just.'
As the clinic teetered on the brink of closing, the community urgently came together to purchase it. Later, when financial difficulties resurfaced, the local government redirected funds from various projects to bolster its finances. Nonetheless, many regular patients—excluding those who are elderly or young—typically pay around A$50 for each visit.
Ms Williams explains that locals end up shouldering the cost of their care thrice—through their Medicare contributions, municipal rates, and finally, the uncovered gap fees.
Who should bear the cost?
"No-one would say this is the Australia that we want, surely," Elizabeth Deveny, from the Consumers Health Forum of Australia, tells the .
Similar to numerous affluent nations, this country is finding it challenging to manage an increasing populace that is generally aging and becoming less healthy.
A growing yet still minor group argues that it might be time to abandon our current understanding of universal healthcare.
A number of physicians, several economists, along with certain conservative political figures have aimed to recast Medicare not as an program for everyone but rather as a protective shield for the country’s most susceptible citizens.
Health economist Yuting Zhang contends that free healthcare and universal healthcare represent distinct concepts.
She points out that the taxes collected by the government for Medicare are far from sufficient to sustain the program. The nation must either engage in difficult discussions about sourcing extra funding or be open to charging higher premiums for those capable of paying more.
Every choice involves a compromise... With finite assets at your disposal, you must carefully consider their optimal utilization.

According to Danielle McMullen from the Australian Medical Association, the initial commitment of Medicare has been "weakened by years of disregard," and many Australians now believe they should bear some responsibility for covering their healthcare costs.
She points out that the freezes on Medicare rebates — which were managed collaboratively by both political parties from 2013 to 2017 and resulted in payment rates failing to match inflation levels — proved too much. As a consequence, numerous physicians have since been covering additional expenses for patients using their personal funds.
The Labor Party and the Liberal-National coalition both acknowledge that there is a crisis, yet they Each one blames the other for causing it.
Opposition leader Peter Dutton says his government will invest A$9bn in health, including funds for extra subsided mental health appointments and for regional universities training key workers.
"Healthcare has emerged as yet another casualty of Labor's cost-of-living crisis... we're aware that it has genuinely never been tougher or pricier to secure an appointment with a general practitioner compared to today’s circumstances," stated health spokesperson Anne Ruston in a press release.
On the contrary, Albanese — frequently pulling out his Medicare card — aims to reassure voters that it was Labor who established this cherished program. He also highlights the Liberal-National coalition’s inconsistent backing of the universal healthcare initiative and Drew Anthony's cost-cutting measures when he served as Health Minister ten years ago.
"At this election, the small card you're holding, your Medicare card, is what's being contested," Albanese has stated.
His government has started fixing things already, he argues, and has pledged an extra A$8.5bn for training more GPs, building additional public clinics, and subsidising more medicines.

However, the main feature of their rescue packages is an enhancement to Medicare rebate rates and larger incentives for physicians who offer bulk billing services.
Suggested initially by Labor and later echoed by the Coalition, these modifications would enable approximately 90% of Australians to visit a general practitioner without any charges, according to both parties.
One Tasmanian doctor tells the it is just a "good election sound bite". He and many other clinicians say the extra money is still not enough, particularly for the longer consults more and more patients are seeking for complex issues.
Labor has little patience for those criticisms, citing research which they claim shows their proposal will leave the bulk of doctors better off and accusing them of wanting investment "without strings attached".
But many of the patients the spoke to are sceptical either parties' proposals will make a huge difference.
They argue that much more needs to be done, listing their desired actions: enhancing efforts to train and retain physicians in rural areas; implementing stricter controls over private healthcare costs along with increased investments in public specialty clinics; providing comprehensive bulk billing coverage for all pediatric medical and dental services; securing additional funds for paramedical professionals and preventive care initiatives.

Experts such as Mr. Breadon argue that, more than anything else, the method of compensating health care providers under Medicare should be revamped to ensure genuine universality in accessing medical services.
That is, the government needs to stop paying doctors a set amount per appointment, and give them a budget based on how large and sick the populations they serve are – that is something several recent reviews have said.
The longer governments delay investing in these reforms, the higher the costs will be.
"The stars might just be aligning now... The time has come for these changes, and postponing them could be extremely risky," states Mr. Breadon.
In Streaky Bay, however, residents such as Ms. Williams question whether it might be too late. The situation has become perilous in this area.
"The maybe it’s just my pessimistic side talking," she remarks, tilting her head.
Universal means everything is equal for all, yet we're aware this isn’t always the case.
- The year the American Dream in Australia came to an end
- Australia's upcoming election highlights the housing crisis.
Further information on the Australian election 2025
- Albanese encounters challenges before the upcoming Australian election.
- In what manner will Australia select its upcoming prime minister?
- Peter Dutton: The Former Police Officer Who Revived Australia's Opposition From the Brink
- Anthony Albanese: The 'Working-Class Hero' Who Lost Popularity